Feeling Fine After 40? Your Blood Pressure May Tell a Different Story
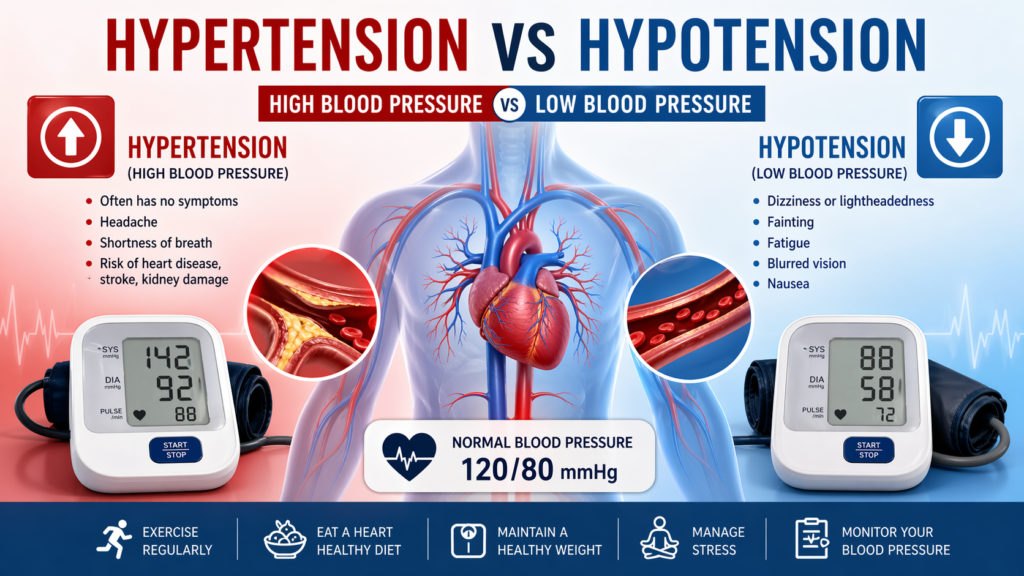
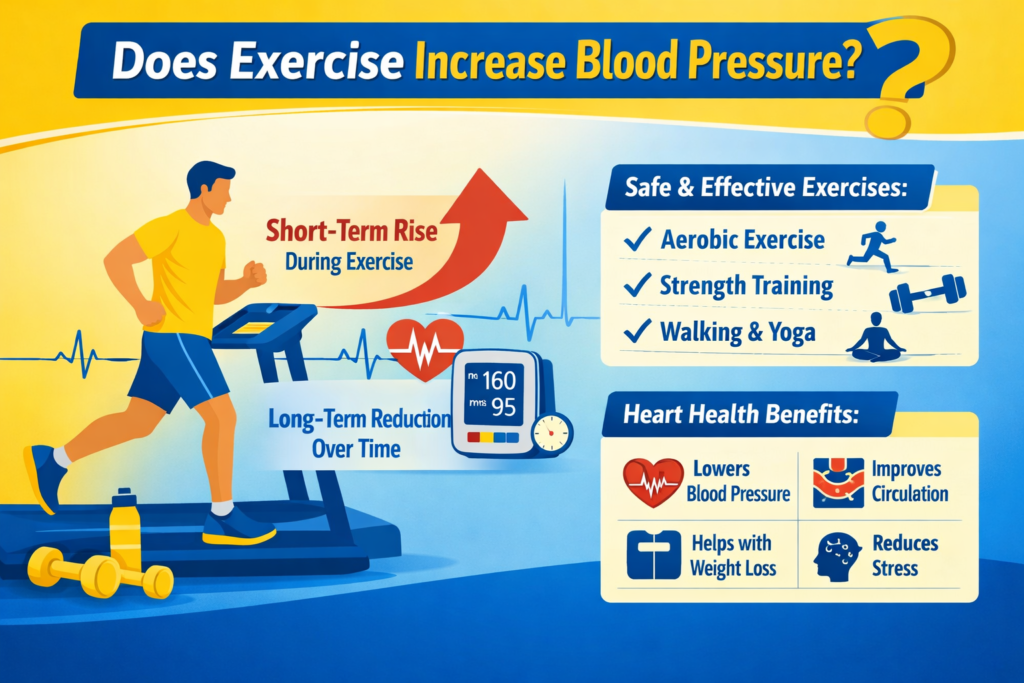
High Blood Pressure With No Symptoms: Why Feeling Fine After 40 Does Not Always Mean Your Blood Pressure Is Healthy Feeling Fine Does Not Always Mean Your Blood Pressure Is Healthy You may feel normal, stay active, go to work, take care of your family, and still have high blood pressure with no symptoms. That is what makes hypertension so easy to miss, especially after age 40. There may be no headache, no dizziness, no chest discomfort, and no obvious warning sign. Why Silent High Blood Pressure Can Still Be Risky But inside the body, silent high blood pressure can quietly place stress on the heart, blood vessels, brain, kidneys, and eyes. The Centers for Disease Control and Prevention notes that high blood pressure is usually defined as blood pressure consistently at or above 130/80 mm Hg, and it often has no signs or symptoms. Why Adults Over 40 in Kingman, AZ Should Pay Attention For adults in Kingman, AZ, especially those with diabetes, obesity, kidney disease, cholesterol problems, heart risk, or Medicare wellness needs, regular blood pressure checks are not just routine. They are one of the simplest ways to detect a problem before it becomes more serious. Blood Pressure Care at Northern Arizona Medical Group At Northern Arizona Medical Group (NAMG) in Kingman, AZ, patients can receive blood pressure evaluation, primary care support, chronic care management, in-house lab testing, and remote patient monitoring when appropriate. NAMG states that it is accepting new patients and offers same-day appointment availability. Why High Blood Pressure Can Be Dangerous Even Without Symptoms Many people expect high blood pressure to “feel” like something. They may wait for symptoms such as headaches, flushing, dizziness, or chest pressure before calling a doctor. The problem is that high blood pressure often does not work that way. The American Heart Association explains that high blood pressure is often called the “silent killer” because there are usually no signs or symptoms, and it needs to be diagnosed in a healthcare setting. That means a person may have hypertension without symptoms for months or years. During that time, the pressure inside the arteries may contribute to long-term damage. High blood pressure can: Make the heart work harder Damage to the arteries over time Increase heart disease risk Increase stroke risk Affects kidney function Contribute to vision problems Worsening risk in people with diabetes or chronic kidney disease This does not mean every high reading is an emergency. It does mean that repeated high readings should not be ignored. Why Adults Over 40 Should Pay Closer Attention Blood pressure often increases with age. The National Heart, Lung, and Blood Institute explains that blood vessels naturally thicken and stiffen over time, which can raise the risk of high blood pressure. After 40, it becomes more important to know your numbers, especially if you have: A family history of hypertension Diabetes or prediabetes High cholesterol Obesity or weight gain Chronic kidney disease Sleep apnea Smoking history Heart disease risk High stress A diet high in sodium Low physical activity For seniors, high blood pressure can also become more complicated because other health conditions, medications, kidney function, and heart health may all need to be considered together. That is why many patients benefit from working with a primary care doctor rather than only checking their blood pressure at home or at a pharmacy once in a while. “I Feel Fine” Does Not Always Mean Your Blood Pressure Is Fine Feeling fine can be reassuring, but it is not a reliable indicator of blood pressure. A person can have hypertension without symptoms and still have elevated numbers. The only way to know is to measure blood pressure correctly and review repeated readings with a healthcare provider. This is especially important for people who say: “I only check my blood pressure when I feel bad.” “I do not have headaches, so I think I am okay.” “My blood pressure was high once, but I felt normal.” “I take medicine sometimes, but not every day.” “I have diabetes, but I do not check my blood pressure often.” If this sounds familiar, it may be time to schedule a blood pressure check in Kingman, AZ. How to Know If You Have High Blood Pressure Start With an Accurate Blood Pressure Reading A blood pressure reading has two numbers: Systolic pressure: the top number Diastolic pressure: the bottom number The American Heart Association lists these general blood pressure categories: Category Systolic Diastolic Normal Less than 120 Less than 80 Elevated 120–129 Less than 80 Stage 1 hypertension 130–139 80–89 Stage 2 hypertension 140 or higher 90 or higher Severe hypertension Higher than 180 and/or higher than 120 These numbers should be interpreted by a healthcare professional, especially if you have diabetes, kidney disease, heart disease, or take multiple medications. Check More Than Once One high reading does not always mean you have chronic hypertension. Blood pressure can rise due to pain, stress, caffeine, exercise, poor sleep, medication effects, or even anxiety during a clinic visit. However, repeated high readings should be reviewed. A primary care provider may recommend: In-office blood pressure checks Home blood pressure logs Medication review Lab testing Kidney function testing Cholesterol testing Diabetes screening or monitoring Heart risk assessment Remote patient monitoring when appropriate How to Check Blood Pressure Correctly at Home Home readings can be helpful, but only if they are done correctly. The CDC recommends steps such as avoiding food or drink for 30 minutes before checking, emptying your bladder, sitting with back supported for at least 5 minutes, keeping your feet flat on the floor, resting your arm at chest height, and placing the cuff on bare skin. For better results: Use a properly sized cuff Sit quietly before measuring Do not talk during the reading Take readings at the same time each day if advised Write down your numbers Bring your log to your appointment Do not change or stop blood pressure medication without talking with your healthcare provider. High
Feeling Fine After 40? Your Blood Pressure May Tell a Different Story Read More »