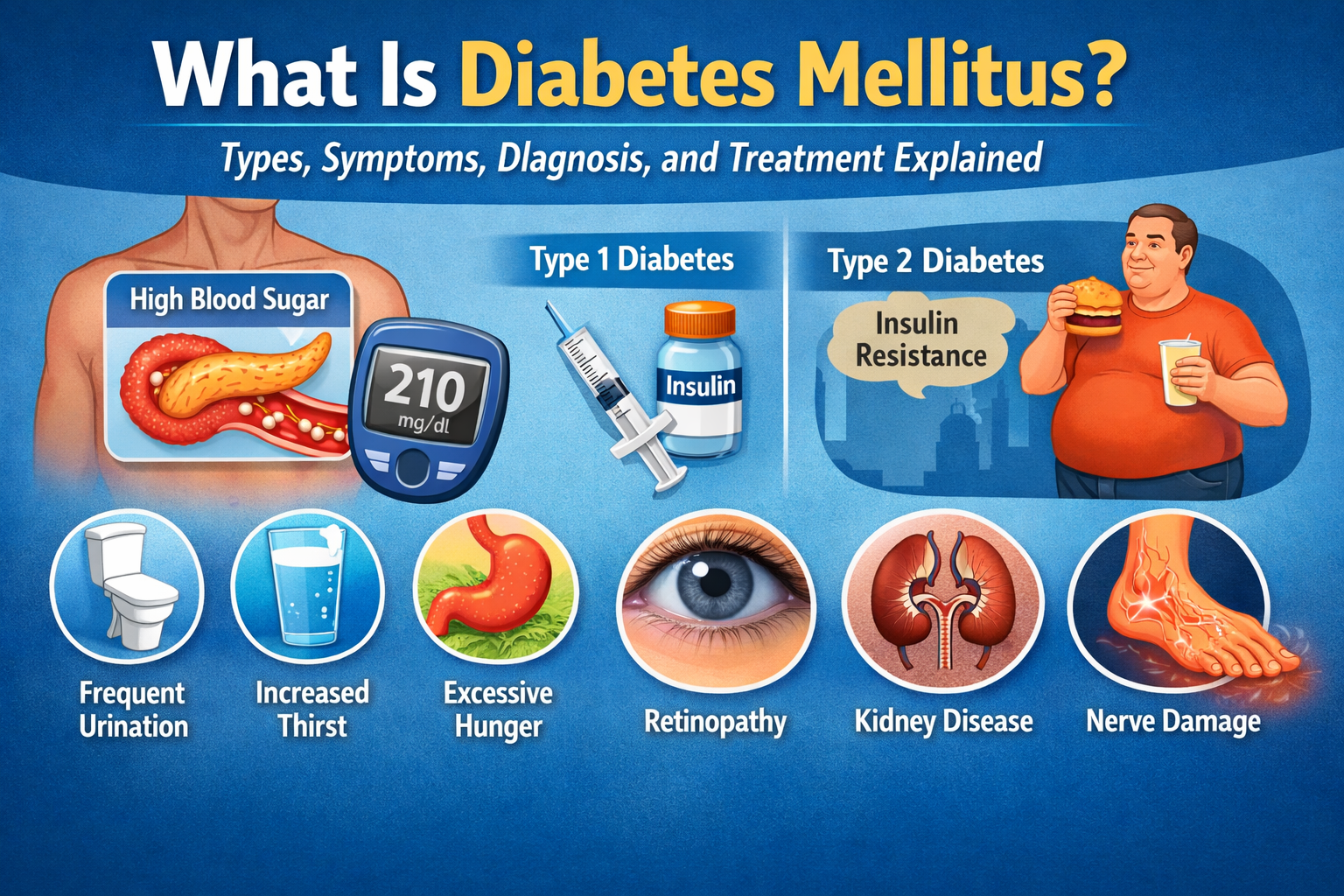
What Is Diabetes Mellitus? A Complete Guide to Types, Symptoms, Diagnosis, and Treatment
Diabetes mellitus is one of the most common chronic health conditions in the world, affecting hundreds of millions of people. Despite being widespread, many people still misunderstand what diabetes actually is, how it develops, and how it can be managed effectively.
In simple terms, diabetes occurs when the body cannot properly regulate blood sugar (glucose) due to problems with insulin production or insulin function.
Understanding diabetes is crucial because early detection and proper management can prevent serious complications such as heart disease, kidney failure, nerve damage, and vision loss.
This comprehensive guide explains everything you need to know about diabetes, including types, symptoms, causes, diagnosis, complications, and treatment options.
What Is Diabetes Mellitus and How Does It Affect the Body?
Diabetes mellitus is a chronic metabolic disorder characterized by elevated blood glucose levels (hyperglycemia).
The condition occurs when:
-
The pancreas does not produce enough insulin, or
-
The body cannot effectively use the insulin it produces.
Insulin is a hormone produced by the beta cells of the pancreas. Its main function is to help glucose move from the bloodstream into cells, where it can be used for energy.
When insulin function is impaired:
-
Glucose builds up in the blood.
-
Cells cannot access energy properly.
-
Long-term damage occurs to blood vessels and organs.
Over time, high blood sugar can damage the:
-
Heart
-
Kidneys
-
Eyes
-
Nerves
-
Brain
-
Blood vessels
How Common Is Diabetes Worldwide?
Diabetes has reached epidemic levels globally.
According to the International Diabetes Federation (IDF) Diabetes Atlas:
-
537 million adults worldwide had diabetes in 2021.
-
By 2030, this number is expected to reach 643 million.
-
By 2045, the number could exceed 783 million people.
Key Global Statistics
-
Nearly 1 in 10 adults worldwide has diabetes.
-
About 240 million people remain undiagnosed.
-
Diabetes causes 6.7 million deaths annually.
Research published in The Lancet Diabetes & Endocrinology indicates that over 90% of cases are type 2 diabetes, largely driven by rising obesity and sedentary lifestyles.
What Are the Main Types of Diabetes?
Diabetes is not a single disease but rather a group of metabolic disorders with different causes and treatments.
The major types include:
-
Type 1 diabetes
-
Type 2 diabetes
-
Gestational diabetes
-
Other specific types of diabetes
Each type has unique characteristics and risk factors.
What Is Type 1 Diabetes?
Type 1 diabetes is an autoimmune disease in which the body’s immune system mistakenly attacks and destroys insulin-producing beta cells in the pancreas.
Because these cells are destroyed, the body cannot produce sufficient insulin.
Key Characteristics of Type 1 Diabetes
-
Usually develops in children, teenagers, or young adults
-
Requires lifelong insulin therapy
-
Accounts for 5–10% of all diabetes cases
Research Insights
Studies show that genetic predisposition combined with environmental triggers, such as viral infections, may contribute to the autoimmune process.
Without insulin treatment, type 1 diabetes can quickly lead to life-threatening complications like diabetic ketoacidosis (DKA).
What Is Type 2 Diabetes?
Type 2 diabetes is the most common form of diabetes and develops when the body becomes resistant to insulin.
Over time, the pancreas cannot produce enough insulin to maintain normal blood glucose levels.
Major Risk Factors for Type 2 Diabetes
Several lifestyle and genetic factors increase risk, including:
-
Excess body weight or obesity
-
Physical inactivity
-
Unhealthy diet
-
Family history of diabetes
-
Aging
-
High blood pressure
-
Polycystic ovary syndrome (PCOS)
Data and Research Findings
Research from the Centers for Disease Control and Prevention (CDC) indicates:
-
90–95% of diabetes cases are type 2.
-
Adults with obesity have up to 7 times higher risk of developing diabetes.
-
Losing 5–7% of body weight can significantly reduce the risk.
Unlike type 1 diabetes, type 2 diabetes usually develops gradually over several years, often without obvious symptoms.
What Is Gestational Diabetes?
Gestational diabetes is a form of diabetes that first appears during pregnancy.
It occurs when pregnancy hormones interfere with insulin action, causing elevated blood glucose levels.
Important Statistics
-
Affects 7–14% of pregnancies worldwide.
-
Usually develops between 24 and 28 weeks of pregnancy.
-
Often disappears after childbirth.
However, gestational diabetes significantly increases long-term health risks.
Long-Term Risks
Research shows:
-
Up to 50% of women with gestational diabetes develop type 2 diabetes within 10 years.
-
Children born to affected mothers have a higher risk of obesity and diabetes later in life.
Are There Other Types of Diabetes?
In addition to the three major forms, several less common types of diabetes exist.
These include:
Monogenic Diabetes
This form is caused by single gene mutations affecting insulin production.
Examples include:
-
MODY (Maturity-Onset Diabetes of the Young)
-
Neonatal diabetes
Monogenic diabetes accounts for about 1–2% of diabetes cases.
Secondary Diabetes
Secondary diabetes occurs as a result of other medical conditions or medications, including:
-
Chronic pancreatitis
-
Pancreatic surgery
-
Cushing syndrome
-
Long-term glucocorticoid therapy
What Are the Early Symptoms of Diabetes?
Diabetes symptoms vary depending on the type and severity of the disease.
In type 1 diabetes, symptoms often appear suddenly and dramatically, while type 2 diabetes may develop slowly over many years.
Common Early Warning Signs
Typical symptoms of diabetes include:
-
Frequent urination (polyuria)
-
Excessive thirst (polydipsia)
-
Increased hunger (polyphagia)
-
Fatigue or weakness
-
Blurred vision
-
Dry mouth
-
Itchy or dry skin
Symptoms Often Seen in Type 1 Diabetes
-
Rapid unexplained weight loss
-
Nausea and vomiting
-
Sudden onset of symptoms
Symptoms Often Seen in Type 2 Diabetes
-
Slow-healing wounds
-
Recurrent infections
-
Tingling or numbness in hands and feet
-
Darkened skin patches called acanthosis nigricans
Hidden Diabetes Risk
Studies suggest that nearly 50% of people with type 2 diabetes remain undiagnosed during early stages because symptoms develop gradually.
How Is Diabetes Diagnosed?
Doctors diagnose diabetes using blood glucose tests.
To confirm the diagnosis, abnormal test results are usually repeated on a different day unless symptoms are clearly present.
Standard Diabetes Diagnostic Criteria
| Test | Diabetes Level | Prediabetes Range | Notes |
|---|---|---|---|
| Fasting Plasma Glucose | ≥126 mg/dL | 100–125 mg/dL | Requires 8-hour fast |
| Oral Glucose Tolerance Test | ≥200 mg/dL | 140–199 mg/dL | After 75g glucose drink |
| Random Plasma Glucose | ≥200 mg/dL | Not applicable | With symptoms |
| HbA1c Test | ≥6.5% | 5.7–6.4% | Reflects 2–3 months average |
Why HbA1c Is Important
The HbA1c test measures average blood sugar over the previous 2–3 months, making it one of the most reliable tools for diagnosing and monitoring diabetes.
What Is Prediabetes?
Prediabetes is a condition in which blood glucose levels are higher than normal but not yet high enough to be diagnosed as diabetes.
Prediabetes Statistics
According to the CDC:
-
1 in 3 adults worldwide has prediabetes.
-
More than 80% of people with prediabetes do not know they have it.
Can Prediabetes Be Reversed?
Yes.
Research from the Diabetes Prevention Program (DPP) shows that:
-
Lifestyle changes can reduce diabetes risk by 58%.
-
Regular physical activity significantly improves insulin sensitivity.
What Complications Can Diabetes Cause?
When blood sugar remains elevated for long periods, it damages blood vessels and nerves throughout the body.
These complications are usually classified as microvascular and macrovascular complications.
What Are the Long-Term Complications of Diabetes?
Diabetic Retinopathy (Eye Disease)
High blood sugar damages the tiny blood vessels in the retina.
Key Facts
-
Leading cause of preventable blindness in working-age adults.
-
About one-third of diabetics develop some form of retinopathy.
Diabetic Nephropathy (Kidney Disease)
Diabetes is the leading cause of chronic kidney disease worldwide.
Approximately 30–40% of diabetic patients develop kidney damage.
Diabetic Neuropathy (Nerve Damage)
High blood sugar damages nerves, especially in the legs and feet.
Symptoms include:
-
Numbness
-
Tingling
-
Burning pain
-
Loss of sensation
Neuropathy increases the risk of foot ulcers and amputations.
Cardiovascular Disease
People with diabetes are 2–4 times more likely to develop heart disease or stroke compared with those without diabetes.
Heart disease is the leading cause of death among diabetics.
What Are Acute Diabetes Emergencies?
Some diabetes complications require immediate medical attention.
Diabetic Ketoacidosis (DKA)
DKA occurs when the body lacks insulin and begins breaking down fat for energy, producing acidic ketones.
Symptoms of DKA
-
Extreme thirst
-
Frequent urination
-
Rapid breathing
-
Fruity-smelling breath
-
Confusion
This condition is most common in type 1 diabetes.
Hyperosmolar Hyperglycemic State (HHS)
HHS usually occurs in type 2 diabetes, particularly in older adults.
Blood sugar levels may exceed 600 mg/dL, leading to severe dehydration and neurological symptoms.
Both DKA and HHS are medical emergencies requiring immediate treatment.
How Is Diabetes Managed and Treated?
Diabetes management focuses on controlling blood sugar levels and preventing complications.
Core Pillars of Diabetes Management
-
Healthy diet
-
Regular physical activity
-
Weight control
-
Blood glucose monitoring
-
Blood pressure and cholesterol management
Research shows that 150 minutes of moderate exercise per week can significantly improve blood sugar control.
How Is Type 1 Diabetes Treated?
Because the body cannot produce insulin, treatment requires lifelong insulin replacement.
Common Treatment Methods
-
Multiple daily insulin injections
-
Insulin pumps
-
Continuous glucose monitoring systems (CGM)
Recent advancements include automated insulin delivery systems, sometimes called artificial pancreas technology.
How Is Type 2 Diabetes Treated?
Type 2 diabetes treatment usually begins with lifestyle modifications.
If blood sugar remains elevated, medications may be prescribed.
Common Diabetes Medications
-
Metformin
-
GLP-1 receptor agonists
-
SGLT2 inhibitors
-
DPP-4 inhibitors
-
Insulin (in advanced cases)
Research shows that early weight loss and lifestyle changes can even put type 2 diabetes into remission in some patients.
What Are the Key Differences Between Type 1 and Type 2 Diabetes?
| Feature | Type 1 Diabetes | Type 2 Diabetes |
|---|---|---|
| Cause | Autoimmune destruction of beta cells | Insulin resistance |
| Typical Age | Childhood or adolescence | Adults (increasing in youth) |
| Body Weight | Usually normal | Often overweight |
| Treatment | Lifelong insulin | Lifestyle + medications |
Why Is Early Detection of Diabetes Important?
Early diagnosis allows individuals to:
-
Control blood sugar levels
-
Prevent complications
-
Improve quality of life
Research shows that early lifestyle intervention can prevent most cases of type 2 diabetes.
Regular screening is especially recommended for people with:
-
Family history of diabetes
-
Obesity
-
Sedentary lifestyle
-
High blood pressure
-
History of gestational diabetes
Final Takeaway
Diabetes mellitus is a complex but manageable condition. With proper education, early diagnosis, and effective treatment, millions of people with diabetes can live healthy and productive lives.
Lifestyle changes, regular monitoring, and modern medical treatments have made it possible to prevent complications and significantly improve long-term outcomes.