Normal Blood Glucose Range: Fasting, After Eating & HbA1c Explained
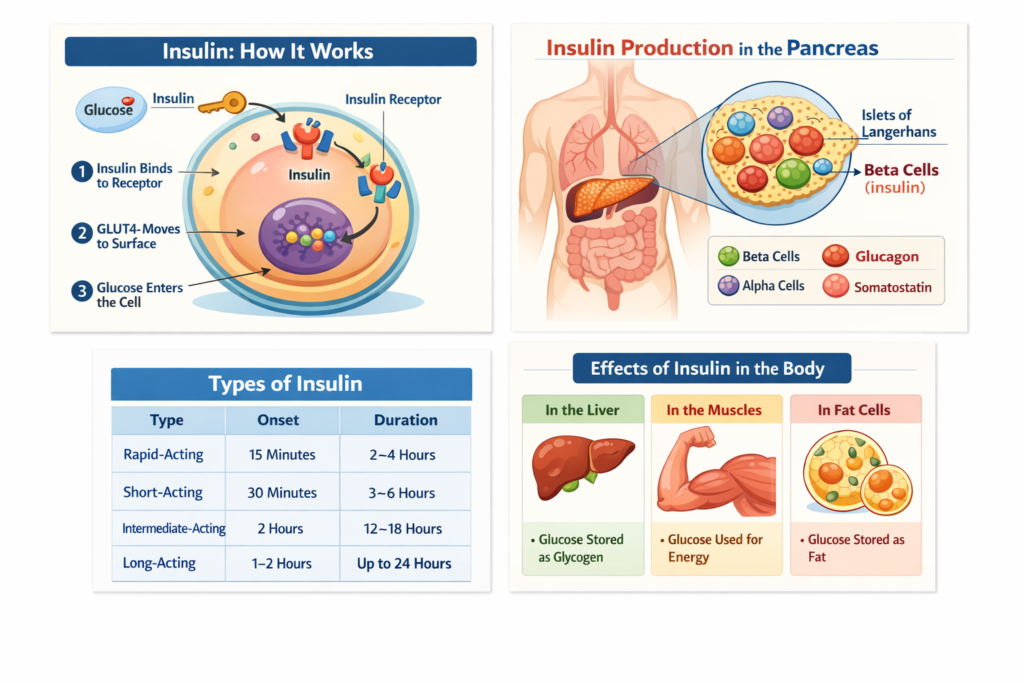
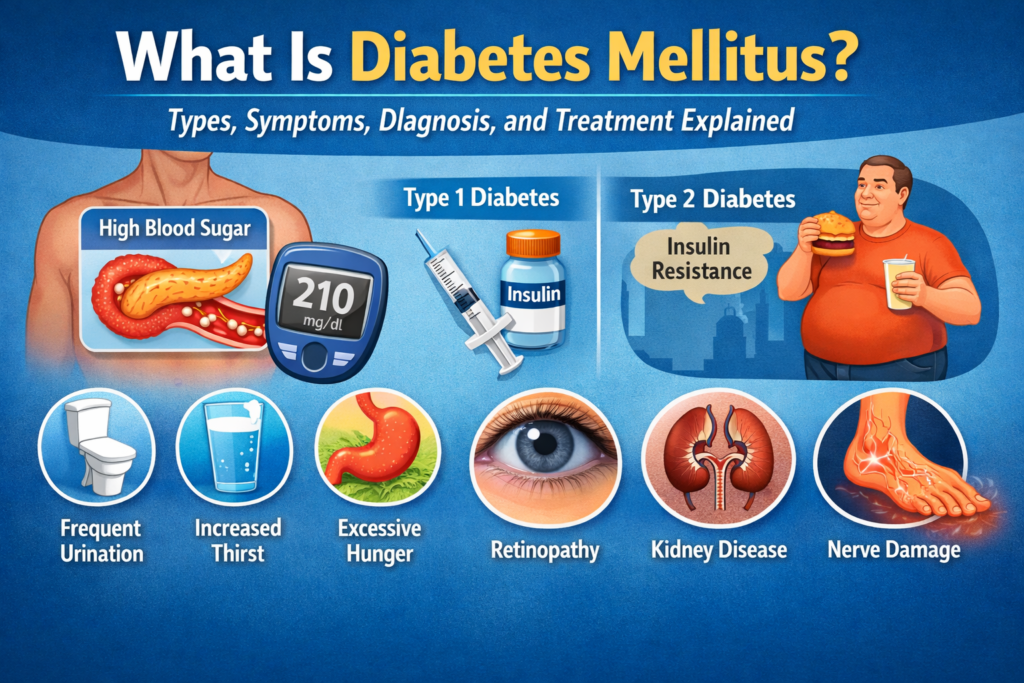
What Is the Normal Blood Glucose Range? Understanding your blood glucose level is one of the most important indicators of your overall health. Whether you’re checking for diabetes, monitoring your diet, or simply being proactive, knowing what “normal” looks like can help you stay in control. The normal blood glucose range for healthy adults is: Fasting: 70–99 mg/dL After eating (2 hours): less than 140 mg/dL Random (any time): usually below 140 mg/dL These values are based on guidelines from trusted authorities like the American Diabetes Association (ADA) and the World Health Organization (WHO). What is blood glucose, and why does it matter? Blood glucose is the amount of sugar (glucose) present in your bloodstream. It is your body’s main source of energy. Glucose comes from: Carbohydrates in food Stored glycogen in the liver Glucose production by the body Your body regulates glucose using insulin, a hormone produced by the pancreas. Why it matters: Too high → risk of diabetes and organ damage Too low → can cause dizziness, confusion, or fainting Stable levels → support energy, brain function, and metabolism What is the normal blood glucose range for healthy adults? Normal blood glucose levels vary depending on timing (fasting, after meals, etc.), but generally stay between 70 and 140 mg/dL. Standard Reference Ranges Condition Normal Range Fasting (8+ hours) 70–99 mg/dL Before meals 70–130 mg/dL 2 hours after meals <140 mg/dL Random <140 mg/dL These ranges apply to individuals without diabetes. What is the normal fasting blood glucose level? A normal fasting blood glucose level is between 70 and 99 mg/dL. Fasting means: No food or drink (except water) for at least 8 hours Why fasting levels matter: They reflect baseline glucose control They are commonly used to diagnose diabetes Interpretation: 70–99 mg/dL → Normal 100–125 mg/dL → Prediabetes 126 mg/dL or higher → Diabetes (confirmed by repeat testing) What is a normal blood sugar level after eating? A normal blood sugar level 2 hours after eating is less than 140 mg/dL. After eating: Glucose rises as food is digested Insulin helps bring levels back down Typical pattern: Peaks within 1 hour Returns to normal within 2–3 hours If levels stay high longer, it may indicate insulin resistance. What is a normal random blood glucose level? A normal random blood glucose level is generally below 140 mg/dL. Random tests: Can be taken at any time Useful for quick screening Important note: A reading of 200 mg/dL or higher, along with symptoms, may indicate diabetes. What are the blood glucose ranges for prediabetes and diabetes? Blood glucose ranges are used to classify metabolic health as normal, prediabetes, or diabetes. Comparison Table Category Fasting (mg/dL) 2-hour OGTT (mg/dL) HbA1c (%) Normal 70–99 <140 <5.7% Prediabetes 100–125 140–199 5.7–6.4% Diabetes ≥126 ≥200 ≥6.5% (Source: American Diabetes Association) What is the HbA1c normal range? A normal HbA1c level is below 5.7%. HbA1c measures: Average blood glucose over 2–3 months Ranges: <5.7% → Normal 5.7–6.4% → Prediabetes ≥6.5% → Diabetes This test is widely used because it reflects long-term control. How do blood glucose levels change throughout the day? Blood glucose naturally fluctuates based on food, activity, and hormones. Typical daily pattern: Morning (fasting): lowest stable level After meals: rises temporarily Between meals: stabilizes Night: may drop slightly Even healthy individuals experience fluctuations. What factors affect blood glucose levels? Multiple internal and external factors influence blood glucose levels. Key factors include: 1. Diet High-carb foods increase glucose quickly Fiber slows absorption 2. Physical activity Exercise lowers blood glucose Improves insulin sensitivity 3. Hormones Insulin lowers glucose Cortisol and adrenaline increase it 4. Stress Emotional or physical stress can raise levels 5. Medications Steroids may increase glucose Insulin lowers it 6. Illness Infection can elevate blood sugar How is blood glucose measured? Blood glucose can be measured using home devices or lab tests. Common methods: 1. Glucometer Finger-prick test Instant results 2. Continuous Glucose Monitor (CGM) Tracks levels throughout the day Useful for diabetics 3. Laboratory tests Fasting plasma glucose (FPG) Oral glucose tolerance test (OGTT) HbA1c Each method provides different insights. What are the symptoms of high and low blood sugar? High and low blood sugar levels produce distinct symptoms. High blood sugar (hyperglycemia): Increased thirst Frequent urination Fatigue Blurred vision Low blood sugar (hypoglycemia): Shaking Sweating Dizziness Confusion Severe cases require immediate medical attention. When should you worry about your blood glucose levels? You should be concerned if your blood glucose consistently falls outside normal ranges. Warning signs: Fasting glucose above 100 mg/dL repeatedly Post-meal levels above 140 mg/dL frequently Random readings above 200 mg/dL Symptoms of hypo/hyperglycemia According to the CDC, approximately 98 million U.S. adults—more than 1 in 3—have prediabetes, and over 80% are unaware of their condition. What are common mistakes when interpreting blood glucose levels? Misinterpreting blood glucose readings can lead to unnecessary worry or a missed diagnosis. Common mistakes: Ignoring timing (fasting vs after meals) Relying on a single reading Not considering symptoms Using outdated reference ranges Self-diagnosing without medical advice Always interpret results in context. Key Takeaways About Normal Blood Glucose Normal fasting glucose: 70–99 mg/dL Normal after meals: less than 140 mg/dL HbA1c normal: below 5.7% Levels vary naturally throughout the day Consistently high or low readings need medical attention Lifestyle plays a major role in glucose control FAQs About Normal Blood Glucose Range What is a dangerously high blood sugar level? A level above 300 mg/dL is considered dangerously high and requires urgent medical attention. Is 110 mg/dL fasting normal? No, 110 mg/dL falls into the prediabetes range. What is normal blood sugar by age? Normal ranges are generally the same for adults, though targets may vary slightly for older individuals. Is a 140 blood sugar after eating normal? Yes, it is the upper limit of normal 2 hours after eating. Can stress raise blood sugar levels? Yes, stress hormones like cortisol can increase blood glucose. How often should I check my blood sugar? If healthy, occasional testing is enough. If diabetic, follow your
Normal Blood Glucose Range: Fasting, After Eating & HbA1c Explained Read More »