What Causes Type 2 Diabetes?
Type 2 diabetes develops when the body becomes resistant to insulin or when the pancreas cannot produce enough insulin to keep blood sugar levels normal. Over time, this leads to high blood glucose levels.
Unlike Type 1 diabetes, which is an autoimmune disease, Type 2 diabetes is strongly influenced by lifestyle, genetics, and metabolic health.
It is also the most common type of diabetes, accounting for about 90–95% of all diagnosed diabetes cases worldwide, according to the Centers for Disease Control and Prevention (CDC).
Understanding what causes Type 2 diabetes can help people identify risk factors early and take steps to reduce their risk.
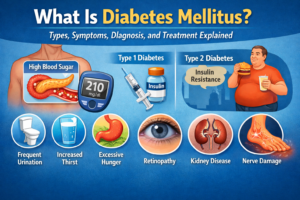
What Is Type 2 Diabetes?
Type 2 diabetes is a chronic metabolic disease that affects how the body regulates blood sugar (glucose).
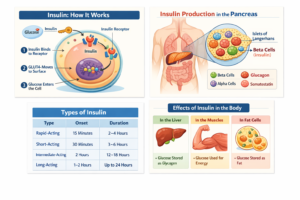
Glucose is the body’s primary source of energy. Insulin, a hormone produced by the pancreas, helps move glucose from the bloodstream into cells.
In people with Type 2 diabetes:
-
Cells become resistant to insulin
-
The pancreas struggles to produce enough insulin
-
Blood glucose levels rise
According to CDC data, about 15.8% of U.S. adults had diabetes between 2021 and 2023, including many undiagnosed individuals.
This makes diabetes one of the most common chronic diseases worldwide.
What Is the Main Cause of Type 2 Diabetes?
The main cause of Type 2 diabetes is insulin resistance combined with declining insulin production.
The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) explains that Type 2 diabetes occurs when the pancreas does not make enough insulin and the body cannot use insulin effectively.
The disease usually develops gradually through several stages:
-
Cells become resistant to insulin
-
The pancreas produces more insulin to compensate
-
Blood sugar begins to rise
-
Insulin production declines
-
Type 2 diabetes develops
This process can occur slowly over many years.
How Does Insulin Resistance Lead to Type 2 Diabetes?
Insulin resistance occurs when cells in the muscles, liver, and fat tissue stop responding properly to insulin.
As a result, glucose remains in the bloodstream instead of entering cells to be used as energy.
The pancreas initially compensates by producing more insulin. However, over time, the pancreas becomes unable to keep up with demand.
Eventually, blood sugar levels increase and Type 2 diabetes develops.
What Is Insulin Resistance?
Insulin resistance means the body’s cells do not respond effectively to insulin’s signal to absorb glucose from the blood.
According to the CDC, when insulin resistance occurs, the pancreas must produce more insulin to maintain normal blood sugar levels.
Over time, this increased demand places stress on the pancreas.
Common contributors to insulin resistance include:
-
Excess body fat
-
Chronic inflammation
-
Physical inactivity
-
Hormonal changes
How Do Cells Become Resistant to Insulin?
Cells become resistant to insulin due to metabolic and hormonal changes that interfere with insulin signaling.
Research suggests several biological factors contribute to this process:
-
Excess abdominal fat
-
Chronic low-grade inflammation
-
Hormonal imbalances
-
Dysfunction in cellular energy systems
These factors reduce the ability of insulin receptors to respond to insulin.
How Do Genetics Influence Type 2 Diabetes Risk?
Genetics plays an important role in determining a person’s risk of developing Type 2 diabetes.
According to NIDDK research, Type 2 diabetes is a polygenic disease, meaning multiple genes contribute to susceptibility.
However, genetics alone does not cause the disease. Lifestyle factors also influence whether diabetes develops.
Is Type 2 Diabetes Hereditary?
Yes. Type 2 diabetes often runs in families.
The CDC identifies having a parent, brother, or sister with Type 2 diabetes as one of the strongest risk factors.
Family members may share both genetic traits and lifestyle habits that influence risk.
Which Genes Are Linked to Type 2 Diabetes?
Researchers have identified several genes associated with increased diabetes risk.
Examples include:
-
TCF7L2 — affects insulin secretion
-
PPARG — regulates fat cell metabolism
-
KCNJ11 — influences insulin release from beta cells
These genes affect insulin production and glucose metabolism.
However, they usually interact with environmental and lifestyle factors.
How Do Lifestyle Factors Contribute to Type 2 Diabetes?
Lifestyle habits strongly influence the development of insulin resistance and Type 2 diabetes.
Key factors include:
-
Excess body weight
-
Lack of physical activity
-
Unhealthy dietary patterns
-
Poor sleep habits
When combined, these factors significantly increase diabetes risk.
Does Obesity Increase the Risk of Type 2 Diabetes?
Yes. Obesity is one of the strongest predictors of Type 2 diabetes.
Excess body fat — particularly around the abdomen — interferes with insulin signaling and increases inflammation.
CDC data show that diabetes prevalence increases significantly as body weight increases.
However, not everyone with obesity develops diabetes, and some people with a normal weight can develop it.
How Does Physical Inactivity Affect Blood Sugar?
Physical inactivity reduces the body’s ability to regulate glucose.
Exercise helps muscles absorb glucose without requiring large amounts of insulin.
According to the CDC, people who are physically active fewer than three times per week have a higher risk of developing Type 2 diabetes.
Regular physical activity improves insulin sensitivity and metabolic health.
Can Diet Increase the Risk of Type 2 Diabetes?
Diet plays a major role in metabolic health.
Long-term dietary patterns that promote weight gain and insulin resistance can increase diabetes risk.
Higher-risk dietary patterns often include:
-
Sugary beverages
-
Highly processed foods
-
Refined carbohydrates
-
Low fiber intake
Healthier eating patterns include:
-
Whole grains
-
Fruits and vegetables
-
Lean protein
-
Healthy fats
NIDDK emphasizes that healthy eating habits are a key part of diabetes prevention.
What Medical Conditions Increase the Risk of Type 2 Diabetes?
Several medical conditions increase diabetes risk because they are closely related to insulin resistance.
Common conditions include:
-
Prediabetes
-
Polycystic ovary syndrome (PCOS)
-
High blood pressure
-
High cholesterol
-
Metabolic syndrome
Prediabetes is especially important because it indicates that blood sugar levels are already higher than normal.
Who Is Most at Risk of Developing Type 2 Diabetes?
Certain groups have a higher risk of developing Type 2 diabetes.
Major risk factors include:
-
Age 45 or older
-
Family history of diabetes
-
Overweight or obesity
-
Physical inactivity
-
History of gestational diabetes
The CDC also notes higher risk among:
-
African American populations
-
Hispanic/Latino communities
-
Native American populations
-
Asian American populations
-
Pacific Islander communities
Can Type 2 Diabetes Be Prevented?
In many cases, Type 2 diabetes can be prevented or delayed through lifestyle changes.
One of the most important studies in diabetes prevention is the Diabetes Prevention Program (DPP).
The study found that lifestyle changes reduced the risk of developing Type 2 diabetes by 58%, while medication reduced risk by 31%.
Effective prevention strategies include:
-
Maintaining a healthy weight
-
Exercising regularly
-
Eating a balanced diet
-
Monitoring blood sugar levels
-
Managing stress and sleep
How Are the Causes of Type 1 and Type 2 Diabetes Different?
| Feature | Type 1 Diabetes | Type 2 Diabetes |
|---|---|---|
| Cause | Autoimmune destruction of beta cells | Insulin resistance |
| Lifestyle influence | Minimal | Major factor |
| Insulin production | Very low or none | Reduced or ineffective |
| Typical onset | Childhood or young adulthood | Usually adulthood |
Key Takeaways
-
Type 2 diabetes develops when the body becomes resistant to insulin.
-
Genetics and lifestyle factors both influence risk.
-
Obesity, inactivity, and diet contribute significantly.
-
Early lifestyle changes can greatly reduce the risk of developing diabetes.
Take Charge of Your Health — Schedule Your Diabetes Consultation Today
If you’re concerned about Type 2 diabetes risk factors, blood sugar levels, or metabolic health, getting professional medical guidance is one of the most important steps you can take. Early screening and personalized care can help detect prediabetes, manage blood sugar, and prevent long-term complications.
At Northern Arizona Medical Group, the healthcare team provides patient-focused care designed to help individuals and families stay healthy. Whether you need a diabetes screening, preventive care, chronic disease management, or a personalized treatment plan, their experienced providers are ready to help.
Why Choose Northern Arizona Medical Group?
-
Comprehensive diabetes screening and risk assessments
-
Personalized treatment and prevention plans
-
Chronic disease management and preventive care
-
On-site diagnostics and lab services
-
Patient-centered care focused on long-term health
Book Your Appointment Today
Don’t wait for symptoms to appear. Early action can make a significant difference in managing and preventing Type 2 diabetes.
Northern Arizona Medical Group
📍 3555 Western Ave
Kingman, AZ 86409
📞 Phone: 928-757-8440
📧 Email: info@namg.us
👉 Call today to schedule an appointment and take the first step toward better health.
Your health matters — and the right medical team can help you protect it.
FAQ
What is the biggest cause of Type 2 diabetes?
The biggest cause is insulin resistance combined with reduced insulin production.
Can eating sugar cause Type 2 diabetes?
Sugar alone does not cause diabetes, but excessive intake can contribute to weight gain and insulin resistance.
Is Type 2 diabetes reversible?
Some people can achieve remission through weight loss, diet changes, and increased physical activity.
What is prediabetes?
Prediabetes occurs when blood sugar levels are higher than normal but not yet high enough for diabetes.
How fast does Type 2 diabetes develop?
It usually develops gradually over many years.